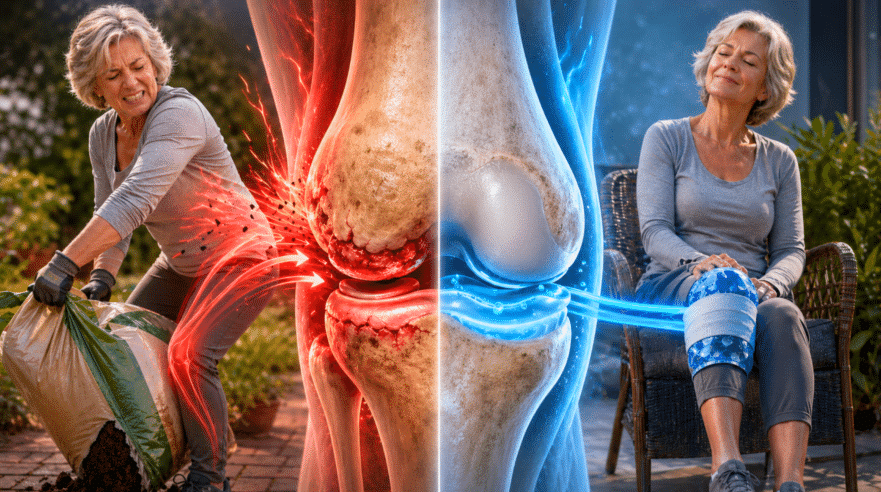
Do you have arthritis in your hips or knees and feel like you’re just not getting it right? Maybe some days are great, but others leave you in agony, wondering what you did wrong. It’s a frustrating cycle, and it can feel like you’re doing everything wrong.
First, let’s reframe the word “mistakes.” It’s a harsh term. Think of these more as common oversights or things you could be doing better to manage your condition. We live in a world where everyone is trying their best, and when you’re in pain, it’s hard to know what the right move is. Based on what we see in our practice every day, we’ve compiled a list of the ten most common things people with hip and knee arthritis do that might be holding them back from feeling their best. This isn’t about blame; it’s about empowerment. By understanding these points, you can take better control of your health, reduce your pain, and keep moving. (Based on the insights of Dr. Paul Zalzal and Dr. Brad Weening)
Key Takeaways
- Avoid the “boom and bust” cycle of activity; aim for consistency.
- Be cautious with pain medications, especially narcotics and long-term NSAID use.
- Give supportive devices like braces, proper shoes, and mobility aids a fair chance.
- Don’t dismiss treatments like injections or physical therapy without a thorough discussion.
- The single biggest mistake is avoiding movement; motion is lotion for your joints.
10. Pushing Through on Good Days: The ‘Boom and Bust’ Cycle
We see this all the time. Your arthritis pain isn’t a constant, stable thing. It waxes and wanes. You wake up one morning and think, “Hey, I feel pretty good today!” That feeling of relief is so powerful that you decide to make up for lost time. You’ll tackle the garden, go for that long walk you’ve been missing, or run all your errands in one go. That’s the “boom.” But what happens the next day? Or for the next six days? It’s a “bust.” You’re in so much pain that you can barely move.
This boom-and-bust pattern is a major pitfall. It creates a vicious cycle of over-activity followed by forced inactivity and pain. The key is to find a middle ground. On your good days, by all means, enjoy being active. But do it mindfully. Instead of walking 10K, maybe walk 5K and take a break in the middle. If you’re gardening, work for 30 minutes and then rest for 15. Pacing yourself is not a sign of weakness; it’s a smart strategy to have more good days and fewer “bust” days. Don’t let one good day ruin your entire week.
9. Relying on the Wrong Pain Pills
When you’re in pain, reaching for a pill seems like the easiest solution. But the type of pill matters—a lot. There are two major errors we see here. The first is using narcotics to manage chronic arthritis pain. Decades ago, this might have been common practice, but we now know the immense dangers. The risk of addiction is incredibly high, as many have learned the hard way. More than that, narcotics don’t solve the underlying problem of inflammation and joint damage. They just mask the pain temporarily. Over time, you need higher and higher doses to get the same effect, and managing your pain after a potential surgery becomes much more complicated. It’s a short-term fix with devastating long-term consequences.
The second error is overusing non-steroidal anti-inflammatory drugs (NSAIDs). These are your common over-the-counter or prescription medications like ibuprofen and naproxen. While they can be effective for short-term flare-ups, using them on a long-term, daily basis is a bad idea. They carry significant risks to your kidneys, your cardiovascular health (heart), and your gut, potentially causing ulcers and bleeding. If you find yourself taking NSAIDs for more than a month straight, it’s time to have a serious talk with your doctor about other, safer strategies. Judicious use is the key.
8. Giving Up on Braces Too Soon
When a doctor suggests a brace, especially for knee arthritis, the reaction is often a quick dismissal. “I’m too proud for that,” “It’s too bulky,” or “I tried it once, and it didn’t work.” This is a mistake. A good brace can be a game-changer. For the knee, an “off-loader” brace can shift pressure away from the damaged part of your joint, providing significant pain relief. This not only helps while you’re active but can also reduce the soreness you feel at the end of the day.
Yes, custom braces can be bulky and expensive, but don’t give up after one try. It can take a couple of weeks to get used to it and see the real benefit. We have patients who love their braces so much they wear them out and come back for another. They can be a fantastic tool to delay the need for surgery. If a custom brace isn’t an option, don’t underestimate simpler solutions. Even a neoprene compression sleeve can provide a sense of support, reduce swelling, and improve your joint awareness (proprioception). Don’t let pride or a single bad experience stop you from trying a tool that could keep you active.
7. Ignoring Your Feet: Bad Shoes and Orthotics
Your entire body is a connected chain, and it all starts at your feet. Wearing the wrong shoes can send shockwaves of force right up to your knees and hips, exacerbating your arthritis pain. What are “bad shoes”? Think flip-flops with zero support, completely flat shoes with no arch, or high heels that throw your entire posture out of alignment. Shoes without adequate cushioning are also a major problem. Every step you take on a hard surface without that buffer is a jolt to your already sensitive joints.
Investing in a good pair of supportive, well-cushioned shoes is one of the simplest and most effective changes you can make. Hand-in-hand with this is considering orthotics. These are custom or over-the-counter inserts for your shoes. For hip arthritis, an orthotic can correct a leg length discrepancy, balancing your pelvis and reducing strain. For knee arthritis, a subtle wedge in an orthotic can help offload the worn-out compartment of your knee. You won’t know if it works until you try, but at the very least, ditch the bad shoes. Your joints will thank you.
6. Saying ‘No’ to Injections Out of Fear
The moment the word “injection” is mentioned, many patients shut down. “No way, I’m not getting a needle in my joint!” The two main objections are fear of pain and fear that the injection will cause more damage. Let’s address these. First, the pain. Yes, a needle has to pass through your skin, so there is a brief moment of discomfort. However, the injection itself, if done correctly, should not be severely painful. The joint is a space; we’re not injecting into a sensitive muscle. If you’ve had a painful experience, it was likely because the needle tip was in the fatty tissue around the joint, which is very sensitive. A simple change in needle direction usually solves this. The brief sting is often well worth the weeks or months of relief that can follow.
Second is the fear that cortisone, a common injection type, is “bad” for you. People worry it will soften their bones or destroy their cartilage. The evidence for this is weak to non-existent, especially when injections are done responsibly—meaning they are spaced out and not done too frequently. A few cortisone shots a year can be an incredibly important tool to break a cycle of inflammation and pain, allowing you to participate in physical therapy and stay active. While there are small risks, like a temporary rise in blood sugar or a very rare risk of infection, these should be weighed against the significant potential benefit. Don’t let fear or misinformation rob you of a potentially effective treatment.
5. Forgetting About Ice
This is one of the easiest, cheapest, and most effective tools in your arthritis-fighting arsenal, yet it’s so often overlooked. After a long day on your feet or a bout of activity, your arthritic joint is likely to be swollen and inflamed. Applying ice is the perfect remedy. Ice helps reduce pain by numbing the area, and it’s a powerful anti-inflammatory, helping to decrease that painful swelling.
Some people worry about getting rid of the fluid, thinking their knee needs it. But when your knee is very swollen, it’s not filled with high-quality lubricating fluid. It’s filled with inflammatory fluid that actually dilutes the good stuff and can be harmful to the joint. Reducing that inflammation is key. All you need is a bag of frozen peas or a gel pack. Just remember to wrap it in a towel—never apply ice directly to your skin for a prolonged period, as it can cause frostbite. Twenty minutes on, twenty minutes off is a great rule of thumb. It’s simple, safe, and it works.
4. Waiting Too Long to Seek Help
“My knee hurts, but I’ll wait until I can’t walk anymore to see a doctor.” This is a very common, and very flawed, line of thinking. Yes, in many healthcare systems, there are unfortunately long wait times to see a specialist and even longer waits for surgery. But that is precisely why you should not wait until the last possible moment. Getting into the system early is crucial.
Seeing your family doctor, a physical therapist, or a surgeon doesn’t mean you’re signing up for surgery that day. It means you’re starting the process. It allows a professional to assess your condition, monitor your progress over time, and, most importantly, offer you all the non-operative treatments we’ve been talking about. You can try injections, bracing, and physical therapy to manage your symptoms and potentially delay surgery for years. It also allows you to establish a relationship with a surgeon, so when the time for surgery does come, you’re not meeting them for the first time when you’re desperate. Don’t wait until your quality of life is zero. Get the ball rolling sooner rather than later.
3. Skipping Physical Therapy and Mobility Aids
This mistake is often rooted in frustration and pride. Many people say, “I tried physical therapy once. It hurt, so I stopped.” This is like trying one dish at a restaurant, not liking it, and swearing off food forever. If your physical therapy program is causing lasting pain, that’s not a signal to quit; it’s a signal to communicate. Tell your therapist! A good therapist will listen and modify your program. The goal is to strengthen the muscles around your joint and improve your mobility, not to cause you more pain. Giving it a real chance is essential.
Tied to this is the reluctance to use a mobility aid like a cane or a walker. Pride is a powerful thing, and many people feel that using a cane is a sign of giving in or looking old. Please, try to look at it differently. Using a cane in the hand opposite your painful hip or knee has been shown to offload that joint by 10 to 20 percent! That’s a huge reduction in force. Walking sticks are just “cool canes” that let you stay more active. A modern walker can have a seat, brakes, and a basket. These aren’t symbols of defeat; they are tools of empowerment that allow you to keep moving, do more, and stay engaged with life.
2. Believing You’re ‘Too Old’ for Help
On an almost daily basis, we see patients, often in their 80s or 90s, who have given up. They come in and say, “I guess I’m just too old to do anything about this arthritis.” This is a heartbreaking misconception. While age is certainly a factor that needs to be considered, especially when discussing major surgery like a joint replacement, it is rarely an absolute “no.” We have patients getting injections at 103 years old!
When it comes to surgery, it’s not about the number; it’s about your overall health, your ability to handle the operation, and your capacity to participate in the recovery. It requires a thoughtful, honest conversation with your family, your doctor, and your surgeon about the risks and benefits. But to simply dismiss all options because of your age is a mistake. You are probably not too old to use ice. You are not too old to use a walker. You are not too old for an injection. And you may not be too old for a life-changing surgery if the potential reward of a pain-free, mobile life outweighs the risks.
1. The Biggest Mistake: Avoiding Movement
If this were a game show, this would be the number one answer on the board. The single biggest mistake people with arthritis make is to stop moving. It’s a logical-sounding trap: “My knee hurts when I bend it, so I’ll just keep it straight. I’ll stay on the couch.” This is the worst thing you can do. Your joints are designed for movement. In fact, arthritis likes movement.
Motion is lotion. The cartilage in your joints doesn’t have its own blood supply; it gets its nutrients from the synovial fluid inside the joint. Movement is what circulates that fluid, bathing the cartilage and keeping what you have left as healthy as possible. When you stop moving, your joint gets stiff, your muscles get weak, and your function plummets. It becomes a downward spiral that is very difficult to escape. Yes, it might be uncomfortable at first, but you have to keep your mobility. Preserving your range of motion is critical, not just for your physical health but for your mental state as well. Remember the old saying, “A rolling stone gathers no moss.” You don’t want your joints to gather moss. You’ve got to move it, move it!
Conclusion
There you have it—the top ten oversights we see in people managing hip and knee arthritis. If you recognized yourself in any of these points, don’t beat yourself up. These are easy and understandable traps to fall into. The goal of this is to provide you with the knowledge to make small, positive changes. By pacing yourself, using the right tools, communicating with your healthcare team, and most importantly, staying active, you can dramatically reduce your pain and improve your function. These adjustments can help you live a happier, healthier, and more mobile life. Remember, you are in charge of your own health.
Source: Dr. Paul Zalzal and Dr. Brad Weening