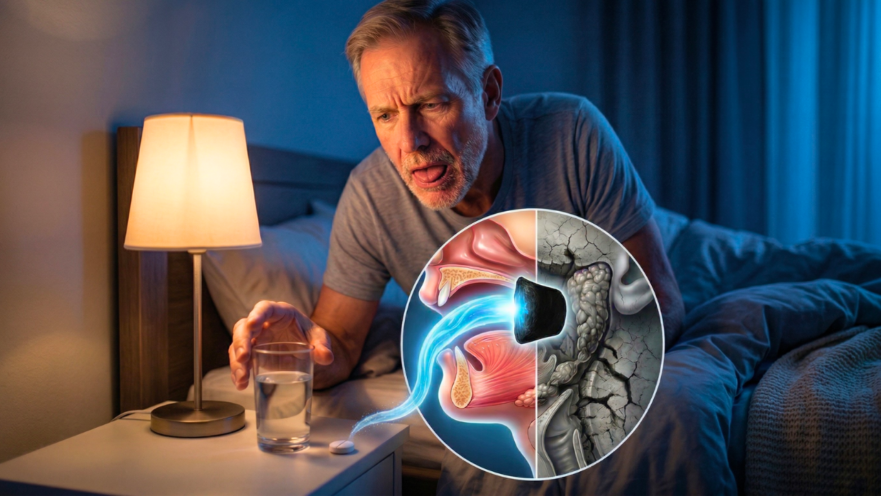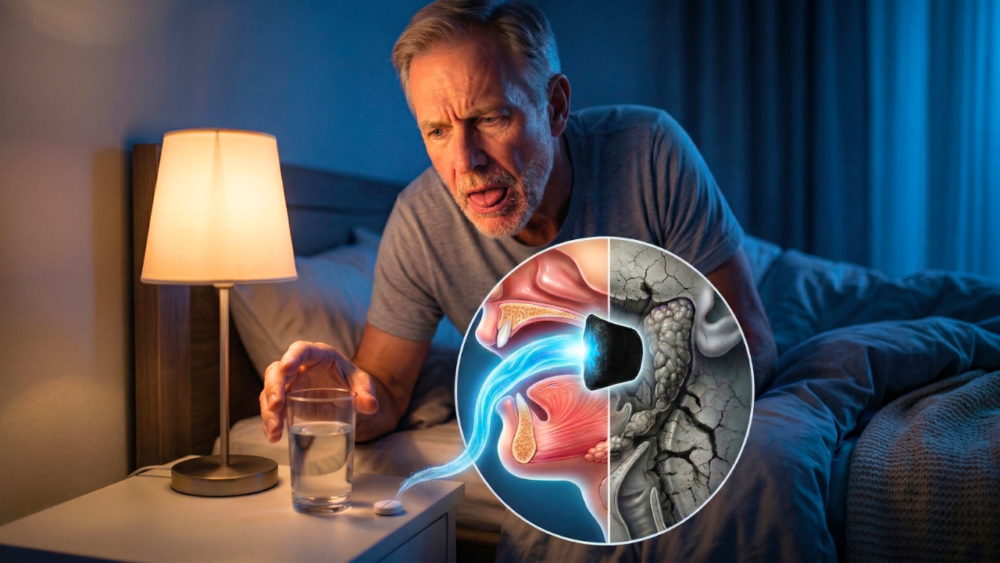
Does this sound familiar? You jolt awake at 3 a.m., your tongue feels like it’s glued to the roof of your mouth, and your whole mouth feels pasty, like you’ve just swallowed a spoonful of sand. Your first instinct is to chug some water, but ten minutes later, that same sandpaper-dry feeling is back with a vengeance. If this is your nightly reality, you’ve probably searched for solutions. You might have even seen the popular advice to drink warm salt water first thing in the morning. Before you try that, please wait. This advice comes with a serious problem. If you’re taking medication for blood pressure, your heart, or even to help you sleep, an extra load of sodium on an empty stomach can be like trying to put out a fire with gasoline—it can make things much worse, especially if you have hypertension or heart failure.
More importantly, that salt water trick doesn’t even address the real problem. To understand what’s happening with your dry mouth, imagine your salivary glands are like automatic sprinklers in a garden. The issue isn’t that the water tank is empty; it’s that someone has cut the wire that tells the sprinklers to turn on. The water is there, but the system isn’t getting the signal to start working. This is precisely what happens to many people over 60 who wake up with a dry mouth. The culprit usually isn’t dehydration, although it can play a role. The real mystery we need to solve is the true underlying cause. (Based on the insights of Dr. Alberto Sanagustín)
Key Takeaways
- It’s Not Just Dehydration: Waking up with a dry mouth is often caused by a signaling problem to your salivary glands, not a lack of water in your body.
- Two Main Culprits: The issue typically stems from either a “chemical blockage” from common medications or a “mechanical blockage” from breathing through your mouth while you sleep.
- Medication Matters: Many common drugs (antidepressants, antihistamines, bladder control meds) have an anticholinergic effect that blocks saliva production. The combined effect of several drugs can be significant.
- Breathing is Key: Nasal congestion or loss of muscle tone can lead to mouth breathing, which evaporates saliva. This can also be a sign of a more serious condition like sleep apnea.
- Actionable Solutions Exist: You can address the root cause by reviewing your medications with your doctor and taking steps to promote nasal breathing during sleep.
1. Understanding Your Saliva’s Night Shift
To figure out why your mouth gets so dry at night, you need to know something that few people realize about their own saliva. Your body doesn’t produce the same kind of saliva at 2 p.m. as it does at 3 a.m. There’s a biological rhythm, a circadian clock, that drastically reduces your saliva production while you sleep. Think of it like a factory that scales down to a skeleton crew for the night shift. It doesn’t shut down completely, but it operates at its absolute minimum. This is perfectly normal.
The problem arises when this natural low point is combined with something else—something that pushes the system even further down when it’s already at its lowest. This “something” can be one of two things, and the solution for you depends entirely on which one it is. The first is a chemical blockage, something that interrupts the nerve signal ordering your glands to produce saliva. The second is a mechanical blockage, something that evaporates what little moisture is left while you sleep. Let’s tackle the first one, as it’s the most common and the most frequently overlooked.
2. Culprit #1: The Chemical Blockage in Your Medicine Cabinet
Remember the analogy of the garden sprinkler with the cut wire? That wire represents your parasympathetic nervous system. Every night, this system sends a signal to your salivary glands via a neurotransmitter called acetylcholine, telling them, “Produce saliva. Keep the mouth moist.” The problem is that a very common group of medications directly blocks this messenger. They don’t do it to annoy you; it’s an unintended side effect of their main function. But the result is the same: the wire is cut, and your glands don’t get the order to produce saliva.
These medications are called anticholinergics, and many people take them without ever knowing they have this effect. The most common ones include:
- Older Antidepressants: Drugs like amitriptyline and clomipramine have a powerful anticholinergic effect. You might be taking them at night for chronic pain or to help with sleep, making them prime suspects.
- First-Generation Antihistamines: Often used for allergies or itching, these can effectively turn off your saliva tap.
- Overactive Bladder Medications: Drugs like solifenacin or oxybutynin act on the same receptors that control saliva. They relax your bladder while simultaneously cutting the signal to your salivary glands.
- Diuretics: Medications like hydrochlorothiazide and furosemide reduce the total volume of fluid in your body. With less available fluid, there’s less available to make saliva, especially at night when you haven’t been drinking for hours.
Are you taking any of these? Here’s something that changes everything: you don’t need to be on one single, powerful drug. Fascinating data reveals that when you combine several drugs that each have a mild anticholinergic effect, the resulting dryness can become severe. Think of it as a shotgun blast instead of a single bullet. One pellet might not do much, but all of them together certainly will. A blood pressure pill might have a mild effect. An occasional antihistamine, a muscle relaxant, a low-dose antidepressant—each one seems innocent on its own. But when you take them all together at night, right when your natural saliva flow is at its lowest, the result is a mouth that feels like cardboard. The sum is often more important than any single part.
3. Culprit #2: The Mechanical Blockage from How You Breathe
The second major culprit isn’t in your pillbox; it’s in how you breathe while you’re asleep. Many people have no idea this is happening to them because they’re unconscious when it occurs. Think about what happens if you leave the refrigerator door cracked open all night. By morning, everything inside will be dried out. It’s not that the fridge stopped working; it’s that air was constantly circulating for hours, ruining the contents. The same thing happens to someone who sleeps with their mouth open. Air flows in and out for seven or eight hours, evaporating every last trace of moisture your glands managed to produce. It doesn’t matter how much water you drink before bed; if you sleep with your mouth open, you will almost always wake up with a dry mouth.
So, why do people sleep with their mouths open? The most common reason is a problem with the nose. You might have a deviated septum, nasal polyps, chronic rhinitis, or allergies. If your nasal passage is obstructed, your body will find the path of least resistance, and that path is your mouth. The second reason, which particularly affects those over 55, is a natural loss of muscle tone in the throat during sleep. The muscles relax more, the jaw drops, and the mouth falls open. This is especially common in people who snore and is also a key sign of sleep apnea. If you’re already using a CPAP machine for sleep apnea, the machine itself can dry out your mouth if the humidifier isn’t adjusted correctly, which is something to discuss with your specialist.
4. How to Tell Which Blockage is Affecting You
So, is your dry mouth caused by a chemical or a mechanical blockage? Ask yourself these questions to find out:
- Do you take two or three (or more) medications on a chronic basis? If so, a chemical blockage from your medications is the primary suspect.
- Do you snore at night or wake up feeling tired and unrefreshed? If yes, the cause is likely mechanical, related to mouth breathing.
- Could it be both? In people over 60, it’s more common than you might think to have a combination of both issues—taking several medications and also snoring or sleeping with your mouth open. Identifying your situation is crucial for figuring out the next step.
5. Your Practical Plan to Combat Dry Mouth Tonight
Now for the good part: what can you actually do about it? Here are two steps you can take starting today, plus an important warning sign to watch for.
Step 1: If You Suspect a Chemical Blockage
Your mission is to review your medication list with your doctor. Never stop or change a medication on your own. This is the most important rule. What you can do is go to your doctor’s appointment prepared with a specific question. Say, “Doctor, I’ve been having severe dry mouth at night. Could any of my medications be causing this?” You could also ask, “Would it be possible to move any of my nightly medications to the morning?” This is a great way to start the conversation. In some cases, the solution might be as simple as changing the time you take a pill, not the dose or the drug itself. The logic is solid: if your saliva factory is already on a skeleton crew at night, it makes no sense to pile on drugs that slow it down even more.
While you wait for that appointment, you can try a couple of over-the-counter remedies. Chewing sugar-free gum, especially gum with xylitol, stimulates your salivary glands and helps protect tooth enamel from cavities—a major risk with chronic dry mouth. You can also try oral moisturizers, which come as sprays or gels from the pharmacy. A sip of water evaporates quickly, but these products are designed to adhere to your oral tissues and provide longer-lasting relief.
Step 2: If You Suspect a Mechanical Blockage
Here, the goal is to get air flowing back through its natural pathway: your nose. Start with a simple saline nasal wash before bed. This can often open up the passages just enough so your body doesn’t resort to mouth breathing. Try sleeping on your side, which reduces the tendency for your jaw to drop open and can also lessen snoring for most people. Placing a pillow between your knees can make side-sleeping more comfortable. If you consistently wake up tired for no reason, snore loudly, or your partner says you stop breathing in your sleep, ask your doctor for a sleep study. Untreated sleep apnea is a serious cardiovascular risk that needs to be ruled out.
6. Red Flags: When Dry Mouth Signals a Deeper Issue
In some situations, dry mouth isn’t just about pills or breathing. It can be a warning sign of an underlying condition that needs medical evaluation. You should see a doctor if:
- Your dryness doesn’t improve after making some of these adjustments.
- You also have persistently dry eyes, which can feel gritty. This could be a sign of Sjögren’s syndrome.
- You experience excessive thirst, frequent urination, and significant fatigue. These are classic symptoms that could point to diabetes.
- You have a history of radiation therapy to the head or neck, which requires specialized management.
This isn’t meant to alarm you, as the vast majority of cases are manageable. But trying to treat only the symptom while the root cause remains active simply doesn’t make sense.
Conclusion: Take Action Tonight
Here is one simple thing you can do today. Tonight, when you take your medications, look at each one and ask yourself three questions: First, do I know exactly what this is for? Second, how long have I been taking it? And third, am I taking this at night because it must be taken at night, or just because I’ve always done it that way? If you don’t have a clear answer to any of these questions, you know what to do: start a conversation with your doctor. Your dry mouth might be the first sign that something is out of balance, and by investigating the cause, you’re taking a powerful step toward better health.
Source: Dr. Alberto Sanagustín