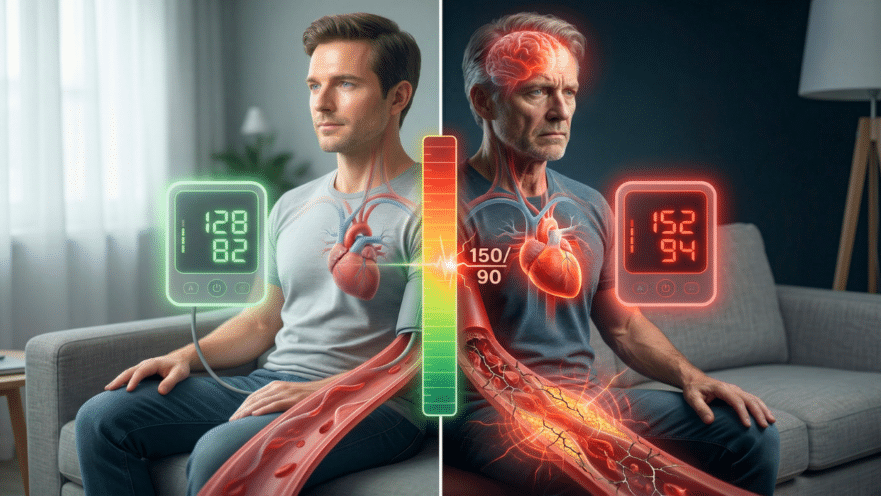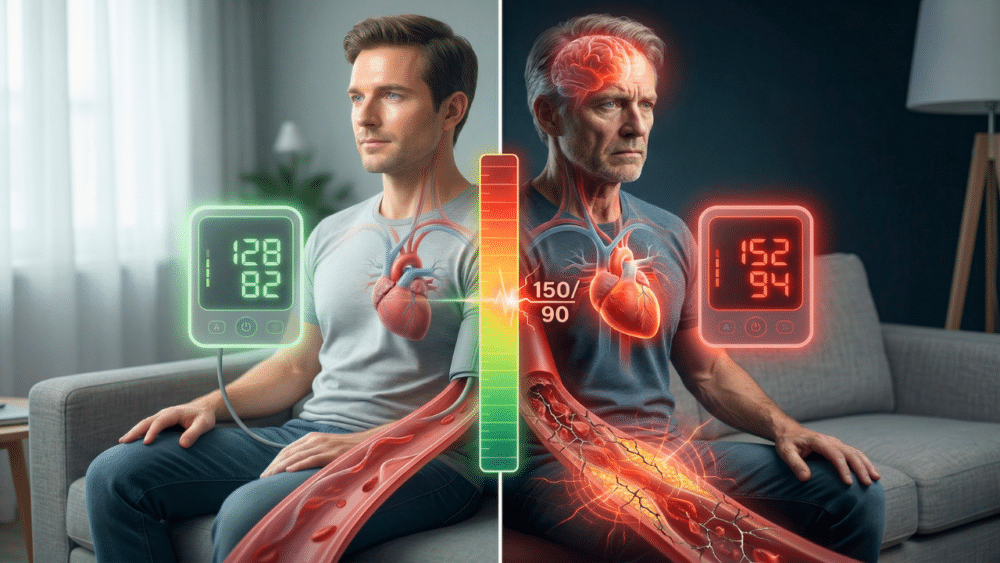
If you want to protect your heart, your brain, and your independence as you get older, you have to understand what your blood pressure numbers really mean. But here’s the problem: most people, especially older adults, have no idea which numbers should truly concern them. You might have been told a high reading is just “normal for your age,” while someone else is told they need another medication for a similar number. It leaves you wondering, is this number dangerous or not?
I understand the hesitation and confusion. The truth is, blood pressure isn’t black and white, particularly as we age. For years, medicine has sent mixed messages. We once thought a systolic pressure of 100 plus your age was normal—meaning a reading of 180 was considered fine for an 80-year-old! We now know that’s too high. But the opposite extreme, aggressively treating every mildly elevated number with medication, isn’t the right approach either. To get clarity, you need to understand what the numbers mean, how your blood pressure behaves in real life, and how to measure it properly. This guide will walk you through exactly that, so you can take control of your health with confidence, not fear. (Based on the insights of Dr. Mitch Rice)
Key Takeaways
- Understand the Two Numbers: Your blood pressure reading has a top number (systolic) and a bottom number (diastolic). The systolic measures pressure when your heart beats, while the diastolic measures pressure between beats. Both are important, but they tell different stories.
- Context is Everything: A single high reading is not a diagnosis. Your blood pressure naturally fluctuates throughout the day with activity, stress, and even just talking. We treat patterns, not single spikes.
- Accurate Measurement is Non-Negotiable: The only way to know your true blood pressure is to measure it correctly and consistently at rest over several weeks. Rushed readings in a doctor’s office or after activity are not your baseline.
- “Too High” Depends on the Pattern: For most people over 60, consistently resting readings above 150 systolic or 90 diastolic are considered too high and require attention. For younger individuals, the threshold is lower (around 140/85).
- Listen to Your Body: Symptoms like shortness of breath, chest pain, or dizziness are red flags, even if your numbers seem borderline. Always consult a professional if you feel unwell.
1. Understanding the Two Numbers: Systolic vs. Diastolic
Every blood pressure reading gives you two numbers, and they measure two distinct moments in your heart’s cycle. The top number is your systolic blood pressure. This is the peak pressure inside your arteries when your heart squeezes to pump blood out. Think of it like a powerful wave hitting the shoreline—it’s the moment of maximum force. As we get older, our arteries naturally become a bit stiffer, so it’s quite common and often normal for this top number to rise slightly over time.
The bottom number is your diastolic blood pressure. This is the pressure in your arteries when your heart relaxes and refills with blood in between beats. It reflects the steady, background pressure your blood vessels are under constantly. This number is less about a peak force and more about the continuous tension in the system. Both numbers matter, but they don’t behave in the same way or always carry the same weight, especially as you age.
2. Decoding Your Systolic (Top) Number
Let’s break down what the top number, your systolic pressure, is telling you. Remember, these are general guidelines, and what matters most is the consistent pattern of your resting blood pressure.
- Below 120: This is considered optimal and ideal for heart health.
- 120 to 129: This is a very acceptable and healthy range.
- 130 to 139: In older adults (over 60), this is often a reasonable range, but only if you feel well and are otherwise healthy. It’s a zone to watch, but not necessarily to treat with medication immediately.
- 140 to 149: This range needs attention. It doesn’t automatically mean you need another pill, but it’s a signal to look closer at your lifestyle, diet, stress levels, and measurement techniques.
- 150 and above: If your blood pressure is consistently 150 or higher at rest, this is something we must take seriously. This level of sustained pressure puts significant strain on your heart, brain, and kidneys.
A key point here is that a systolic reading in the 130s or low 140s, especially in someone over 60 who feels well and is active, is not an emergency. What truly matters is how often you see these readings, how high they go, and under what conditions.
3. Decoding Your Diastolic (Bottom) Number
Now for the bottom number, your diastolic pressure. This number reflects the constant strain on your arteries, so a persistently high reading is a significant concern.
- Below 80: This is generally ideal.
- 80 to 84: This is very common and usually fine.
- 85 to 89: This is a sign that I’d want to watch your blood pressure patterns closely over time.
- 90 and above: A diastolic pressure that is consistently 90 or higher at rest deserves serious attention. This indicates that your arteries are under constant high pressure, even when your heart is relaxed, which can lead to damage over time.
So, when you put it all together, consistently having resting numbers of 150-plus systolic and/or 90-plus diastolic is what I consider to be too high for most people.
4. The Golden Rule: Why “At Rest” is Non-Negotiable
The most important part of this entire process—and the one most people miss—is that these numbers must be taken at rest. The only way you can truly tell if your blood pressure is too high is by getting accurate, consistent readings when your body is completely calm over a period of weeks. A reading of 150 taken in the middle of a stressful workday after you rushed to an appointment is not your true blood pressure; it’s your reactive blood pressure. The timing and the method you use to measure your blood pressure matter more than anything else.
5. How to Measure Your Blood Pressure Accurately at Home
To find your true baseline, you need to follow a strict protocol every single time you measure. This removes the variables that can give you a falsely high reading. Here’s what you need to do:
- Sit Quietly: Before you even touch the cuff, sit in a comfortable chair with your back supported for five full minutes. No talking, no scrolling on your phone.
- Get Positioned: Place both feet flat on the floor (don’t cross your legs). Rest your arm on a table or armrest so that the cuff will be at the same level as your heart.
- Empty Your Bladder: A full bladder can actually raise your blood pressure reading by several points.
- Take Two Readings: Take one measurement. Wait one minute, then take a second one.
- Record the Lower Number: Of the two readings you just took, write down the lower one. This is your reading for that session.
It’s also essential to use a reliable, validated upper-arm blood pressure cuff. Do this routine twice a day: once about 20 minutes after you wake up and again as the last thing you do before bed. Alternate arms each day. After one week, you will have 14 readings. Average those numbers together, and that is your true baseline blood pressure.
6. Your Blood Pressure’s Daily Dance: Why Spikes Happen (and Why You Shouldn’t Panic)
This point is huge, so please hear me out. Your blood pressure is not a fixed number. It is designed to go up and down throughout the day, sometimes by 20 to 40 points or more. This is normal physiology, not a disease. Your blood pressure naturally rises with movement, stress, pain, excitement, caffeine, cold weather, or even just talking. It naturally falls with rest, sleep, calm breathing, and warmth. This is why a reading of 145 at noon during a busy day and 126 in the evening while relaxing on the couch can both be perfectly normal for you. We do not treat single spikes; we treat sustained patterns. I myself have a resting blood pressure around 120/80. But if I were chasing my dog around the house and then stubbed my toe, it would easily jump to 150 systolic, and that would be a completely normal reaction.
7. When to Pause Before Adding Another Pill
Understanding that blood pressure fluctuates is why I often pause before immediately adding a new medication, especially in older patients. I slow down and investigate further in these situations:
- If blood pressure only rises during stressful events (like a doctor’s visit, known as “white coat hypertension”).
- If readings are consistently normal when measured properly at home.
- If high numbers quickly drop back to normal with a few minutes of rest.
- If the person feels well overall and has no symptoms.
- If the person is at risk for falls or already experiences dizziness, as lowering their pressure too much could be dangerous.
In these cases, focusing on lifestyle factors like improving sleep, managing stress, gentle movement, and diet can often be more effective and safer than another prescription.
8. Red Flags: When High Blood Pressure is a Serious Concern
While we don’t panic over single high readings, there are certain situations where my threshold for concern becomes lower and I consider blood pressure to be too high even at slightly lower numbers. These red flags include:
- Delayed Recovery: If your blood pressure stays high for a long time after exercise and doesn’t come down.
- Existing Conditions: If you have known kidney disease, a prior stroke, or heart disease.
- Concerning Symptoms: If elevated readings are accompanied by symptoms like chest pain, shortness of breath, severe headache, or visual changes.
The bottom line is that I am treating the person in front of me, not just the numbers on a screen. Your overall health picture dictates the right course of action.
Conclusion: Take Control Through Understanding
If you remember anything from this guide, let it be this: your blood pressure moves throughout the day, and that’s normal. The key is to measure it correctly at rest, look for consistent patterns over time, and not panic over a few high numbers. Not every elevated reading needs medication. Some numbers are indeed too high and require action, but many are just signals from your body, not emergencies. By understanding what your blood pressure is telling you, you can replace fear with control. And that is the number one goal for your long-term health and well-being.
Source: Dr. Mitch Rice